Philip Yen, MD
- Department of Diagnostic Imaging
- UC Davis Medical Center
- Sacramento, California
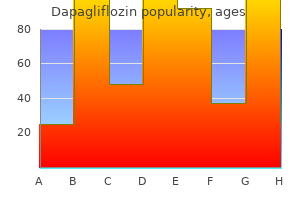
The stent retriever can be withdrawn and reinserted until reperfusion is satisfactory diabetic coma buy 10 mg dapagliflozin amex. In addition diabete type 1 cheap dapagliflozin 10mg online, there was no involvement of anesthesiologists in either the trials or the resulting papers diabetes symptoms in children under 2 10mg dapagliflozin with visa. Two practice workflow and anesthesia surveys from the United States and Scandinavia were published in 2017 blood sugar control yoga buy cheap dapagliflozin 5mg line. Dexmedetomidine and propofol may both cause hypotension diabetes prevention harvard cheap dapagliflozin 10 mg, but dexmedetomidine use requires higher doses of vasopressors. A small dose of fentanyl before deployment of the stent retriever and each withdrawal is helpful. They will be institutionspecific as they draw on the available resources and expertise. Early extubation and strict adherence to neurological protocols restricting oral intake until competent swallowing is demonstrated prevents postoperative pneumonia and improves stroke outcomes. Depressed consciousness, agitation, and risk of aspiration require general anesthesia with endotracheal intubation. Cooperative patients may be managed with local anesthesia only or with mild sedation. These findings are preliminary and may not be generalizable to all centers and all practice types. In light of the newest studies, intraarterial (endovascular) treatment (thrombectomy) for acute ischemic stroke can be performed until 24 hours after stroke onset. Select the most appropriate statement: a) False, the cutoff for treatment is 6 hours. Hypotension is a highly undesirable hemodynamic change, which may be responsible for poor neurological outcomes. Although seizures are a known complication of reperfusion after carotid endarterectomy, in the setting of acute ischemic stroke intracerebral hemorrhage is the most feared and life and function-threatening complication. Because of disruption of the blood-brain barrier in areas that were ischemic, hemorrhage is likely. There is recognition that hypocapnia may contribute to the poorer neurological outcomes associated with general anesthesia; one of the modifiable elements of management which may contribute to hypoperfusion of the ischemic areas of the brain is hypocapnia. All the randomized controlled trials focused on maintaining normoventilation and general anesthesia did not result in worsened neurological outcomes. This is a routine value that neurologists always obtain as part of the basic stroke work-up. In the randomized controlled trials comparing general anesthesia and sedation for stroke, many patients were excluded from randomization because of vomiting, agitation or impending respiratory compromise. The procedure is performed on a horizontal table with the head restrained, greatly increasing the risk of aspiration if vomiting occurs. Society for Neuroscience in Anesthesiology and Critical Care Expert Consensus Statement: anesthetic management of endovascular treatment of acute ischemic stroke. Anesthetic management and outcome in patients during endovascular therapy for acute stroke. Type of anesthesia and differences in clinical outcome after intra-arterial treatment for ischemic stroke. Effect of general anesthesia on functional outcome in patients with anterior circulation ischaemic stroke having endovascular thrombectomy versus standard care: a meta-analysis of individual patient data. Anesthesia practices for endovascular therapy of acute ischemic stroke: a Nordic survey. Wide variability in prethrombectomy workflow practices in the United States: a multicenter survey. Safety and hemodynamic profile of Propofol and Dexmedetomidine anesthesia during intra-arterial acute stroke therapy. Even small decreases in blood pressure during conscious sedation affect clinical outcome after stroke thrombectomy: an analysis of ischemic thresholds. Effect of conscious sedation vs general anesthesia on early neurological improvement among patients with ischemic stroke undergoing endovascular thrombectomy: a randomized controlled trial. General anesthesia versus conscious sedation for endovascular treatment of acute ischemic stroke: the AnStroke Trial (anesthesia during stroke). Effect of general anesthesia and conscious sedation during endovascular therapy on infarct growth and clinical outcomes in acute ischemic stroke: a randomized controlled trial. The daughter reports at least two previous occasions during the past 6 months when her mother suddenly felt "weak" and out of balance but that the symptoms disappeared shortly after their onset. The procedure proves difficult, and the neurosurgeon decides that open surgery is required. Microvascular anastomoses, on the other hand, are low-flow bypasses, also known as "indirect. Direct bypass retains a high patency rate at the added risk of hyperperfusion syndrome. As such, avoiding sharp spikes or drops in hemodynamics at induction, intubation, and surgical incision is a must. This can ensure early detection of hypotension in patients at risk of ischemia from reduced perfusion and hypertension in patients with aneurysms at risk for rupture. In addition, central venous access should be considered in patients with comorbidities, especially those anticipated to require vasopressor administration. The benefit here is twofold: the clinician can estimate the extent of local involvement as well as establish a baseline of symptoms against which all postoperative assessments will be compared. Alternatively, these patients may be otherwise healthy and in their early stages of life. Medical management of co-existing diseases (cardiovascular, pulmonary, endocrine, or otherwise) should be maintained per institutional guidelines. A multidisciplinary team is ideal in dealing with the ramifications of individual diseases and can ensure a safer process overall. Preoperative workup should include all the investigations normally recommended for a craniotomy. If the bypass is being done to circumvent an aneurysm, a gradual and slow induction is required to avoid severe hypotension or hypertension and rapid changes in aneurysmal transmural pressure which may lead to rupture and fatal bleeding. Typical drugs used include phenylephrine and ephedrine to treat hypotension, and barbiturates, opioids, blockers, or a combination of those to treat hypertension. Attention should be given to patients with comorbid conditions such as coronary artery disease or heart failure where coronary perfusion is crucial and episodes of severe or prolonged hypotension may precipitate myocardial injury. The existence of systolic and/or diastolic dysfunction necessitates careful titration of anesthetic agents with cardiodepressive effects, such as propofol and inhalational agents. Maintenance of general anesthesia should aim at achieving a steady state of hemodynamics as rapidly as possible. The use of an inhalational agent coupled with continuous short-acting analgesia with or without barbiturates can be an option. A continuous infusion of a neuromuscular blocking agent is also considered routine in several centers. A temporary clip is sometimes placed on a major feeding artery during anastomosis and can cause a dramatic decrease in blood flow to an area as large as an entire hemisphere. The surgeon will try to minimize the time spent during the temporary clip phase, but a few seconds may be enough to induce considerable damage. Hyperventilation may cause vasoconstriction, thus normocarbia is encouraged in these procedures. Too low Risk of complications Ischemia High risk Bleeding Moderate risk Lowest risk Blood pressure Blood pressure management and the risk of complications during surgery. Ideal hemodynamic management aims at maintaining blood pressure in the safe zone and avoids the risks of bleeding or ischemia with hypertension and hypotension, respectively. The lowest risk zone revolves around a theoretical blood pressure range that is set based on patient characteristics and surgical findings. A severe drop in blood pressure greatly increases the risk of hypoperfusion and brain ischemia, whereas a sharp increase in blood pressure predisposes to bleeding and worse outcomes. Any acute change in mentation or abrupt development of symptoms warrant emergent evaluation by the caregiver team. Hence, these patients are placed in high-acuity monitoring areas (such as a neurointensive care unit). Decreasing cerebral blood flow would lead to ischemia, especially in the penumbra. The following is false regarding Moyamoya disease: a) Risk is increased with family history. Moyamoya (Japanese for "puff of smoke") is a progressive arterial stenosis leading to the formation of multiple thin collaterals. It is more commonly seen in families of affected individuals, although any condition that leads to neovascularization could potentially give rise to a similar picture. The most common presenting symptom in the pediatric age group is cerebral ischemia, while bleeding is the more common presenting symptom in adults. A meta-analysis in 2008 concluded the overall safety of the procedure,14 but other studies have attempted to classify outcome based on preexisting patient characteristics. This can include hypoperfusion of the ophthalmic artery region leading to blindness. Such complications can be detected through continuous monitoring and clinical examination. An abrupt bleeding or thrombosis may manifest as a sudden headache or a new focal neurological deficit. Which of the following is not associated with increased risk of a cerebral ischemic event All the above are risk factors for cerebral ischemic events, systemic hypertension being the most significant. Open surgical treatment of an intracranial aneurysm is indicated when endovascular treatment is not possible (bleeding) or not feasible (larger sized aneurysms, complex structure, or hard to reach intravascularly). At which cerebral blood flow threshold is the electrical activity of the brain lost Which of the following medications and agents has the least effect on cerebral autoregulation While the exact effects of nitrous oxide are not fully understood, it affects cerebral blood flow less than other inhalational agents and has a minimal effect on cerebral autoregulation. Barbiturates and opioids decrease cerebral perfusion via cerebral vasoconstriction. The patient may be placed on a continuous aspirin regimen with daily neurological evaluation as well as cerebral blood flow testing via flow Doppler sensors. Any acute change in mentation or abrupt development of symptoms warrants emergent evaluation by the caregiver team. Ketamine is not routinely used due to its resultant increased cerebral pressures and metabolic demands. Extracranial to intracranial bypass for the treatment of cerebral aneurysms in the pediatric population. Extracranial-intracranial arterial bypass surgery for occlusive carotid artery disease. Microsurgical anatomy of the infratemporal fossa as viewed laterally and superiorly. Posterior auricular artery as an alternative donor vessel for extracranial-intracranial bypass surgery. Bypass surgery for complex middle cerebral artery aneurysms: an algorithmic approach to revascularization. Anesthetic management of the adult patient with concomitant cardiac and pulmonary disease. Predicting cerebral hyperperfusion syndrome following superficial temporal artery to middle cerebral artery bypass based on intraoperative perfusion-weighted magnetic resonance imaging. On exam, her primary care doctor noted numbness on the lateral aspect of the patient right hand. The patient is referred to a spinal surgeon who confirmed the finding of the primary care doctor. Additionally, the patient now complains of shooting pain down her right upper extremity with electric shocks into her right hand with neck extension. The patient denies any improvement with physical therapy, oral corticosteroids, or pregabalin. The surgeon wants to realign the neck prior to instrumentation, detaches the Mayfield head holder from the table, and resets the neck angle. At the end of the procedure, the patient is turned supine and the Mayfield pins are detached. Her postoperative neurological exam is at baseline, but she complains of significant neck pain. After induction and intubation, the patient is placed in Mayfield pins and positioned prone.
Ulnar Artery Ulnar recurrent artery Anterior ulnar recurrent artery Posterior ulnar recurrent artery Common interosseous artery Anterior interosseous artery Median artery Posterior interosseous artery Perforating branch Recurrent interosseous artery Dorsal carpal branch Palmar carpal branch Deep palmar branch Superficial palmar arch Common palmar digital arteries (3) Proper palmar digital arteries 7 diabetes mellitus nursing care plans pdf order dapagliflozin now. Radial Artery Radial recurrent artery Palmar carpal branch Superficial palmar branch Dorsal carpal branch Dorsal carpal arch Dorsal metacarpal arteries Dorsal digital arteries Princeps pollicis artery Radialis indicis artery Deep palmar arch Palmar metacarpal arteries Perforating branches Superior thoracic a managing type 1 diabetes in adults order 10mg dapagliflozin fast delivery. Pectoral branch Clavicular branch Acromial branch Deltoid branch Thoracoacromial a type 2 diabetes quality of life purchase online dapagliflozin. Level of lower margin of teres major muscle is landmark for name change from axillary to brachial a diabetic stroke buy dapagliflozin 5 mg line. Superficial palmar arch *Direction of blood flow is from top (proximal) to bottom (distal) diabetes mellitus type 3 cheapest generic dapagliflozin uk. Brachial Vein(s) Subscapular vein Circumflex scapular vein Thoracodorsal vein Superficial Veins Palmar digital veins Superficial palmar arch Metacarpal/carpal tributaries Dorsal venous network of hand Basilic vein of forearm Cephalic vein of forearm Median vein of forearm Median cubital vein 1. Basilic hiatus *Direction of blood flow is from distal (hand) to proximal (heart). Dorsal venous network (dorsal surface) Deep palmar venous arch Palmar metacarpal vv. The median cubital vein, often coursing between the cephalic and basilic veins in the cubital fossa, is often accessed for venipuncture to withdraw a blood sample. Even the axillary vein usually consists of multiple veins surrounding the single axillary artery. The axillary vein(s) then drains into the subclavian vein (5) on each side (right and left). The subclavian vein(s) then drains into the left and right brachiocephalic veins (6), which drain into the superior vena cava (7) and then the heart (right atrium) (8). In the human body the venous system is the compliance system, and at rest about 65% of the blood resides in the low-pressure venous system. Veins generally are larger than their corresponding arteries and have thinner walls, and multiple veins often accompany a single artery; the body has many more veins than arteries, and veins are more variable in location than most arteries. Pain Compression of suprascapular nerve may cause lateral shoulder pain and atrophy of supraspinatus and infraspinatus muscles Musculocutaneous nerve Musculocutaneous nerve compression within coracobrachialis muscle causes hypesthesia in lateral forearm and weakness of elbow flexion Hypesthesia Coracobrachialis m. It also conveys cutaneous sensory information from the posterior forearm and the radial side of the dorsum of the hand. The radial nerve is vulnerable in fractures of the humeral midshaft or by compression injuries of the arm. It also is vulnerable to compression in the forearm because the deep branch of the radial nerve passes through the two heads of the supinator muscle. The superficial branch of the radial nerve is sensory and may be injured at the wrist. Median Nerve in Forearm and Hand the median nerve (C6, C7, C8, T1) innervates all the muscles of the forearm anterior compartment (wrist and finger flexors and forearm pronators) Chapter 7 Upper Limb 419 7 Clinical Focus 7-22 Radial Nerve Compression Motor signs Provocative tests for radial tunnel syndrome Resistive extension of middle finger Posterior interosseous syndrome Proximal compression; loss of wrist and finger extension (wrist drop) Provocative tests elicit pain over radial tunnel. Sensory signs in radial tunnel syndrome Pain and tenderness Pain radiation Paresthesia and hypesthesias Compression site Proximal Etiology and effects Humeral fracture, tourniquet injury, or chronic direct compression (Saturday night paralysis); weakened elbow, wrist, and finger extension, and supination Repetitive forearm rotation or fracture; posterior compartment neuropathies and radial tunnel syndrome Trauma, tight handcuffs, cast, or watchband; paresthesias in dorsolateral aspect of hand Radial n. Chapter 7 Upper Limb Posterior view Extensor-supinator group of muscles Posterior interosseous n. The median nerve also innervates the thenar muscles and first two lumbrical muscles in the hand. Although well protected in the arm, the median nerve is more vulnerable to traumatic injury in the forearm, wrist, and hand. Entrapment at the elbow and wrist may occur, and the recurrent branch of the median nerve on the thenar eminence may be damaged in deep lacerations of the palm. Ulnar Nerve in Forearm and Hand the ulnar nerve (C7, C8, T1) innervates the flexor carpi ulnaris muscle and the ulnar half of the flexor digitorum profundus muscle in the anterior forearm and most of the intrinsic hand muscles: hypothenar muscles, two lumbricals, adductor pollicis muscle, and all of the interossei muscles (palmar and dorsal). The ulnar nerve is vulnerable as it passes posterior to the medial epicondyle of the humerus; blunt trauma here can elicit the "I hit my funny bone" tingling sensation. The ulnar nerve is also vulnerable as it passes through the two heads of the flexor carpi ulnaris muscle and the cubital tunnel beneath the ulnar collateral ligament. At the wrist, the nerve is vulnerable in the ulnar tunnel, where it passes deep to the palmaris brevis muscle and palmar (volar) carpal ligament, just lateral to the pisiform bone (Clinical Focus 7-24). Abductor pollicis brevis Opponens pollicis Superficial head of flexor pollicis brevis (deep head often supplied by ulnar n. Repetitive forearm pronation and finger flexion, especially against resistance, can cause muscle hypertrophy and entrap the nerve. Pronator syndrome Hypesthesia and activity-induced paresthesias Pain location Provocative maneuvers Compression by flexor digitorum superficialis m. Pronation against resistance Compression by bicipital aponeurosis Flexion of wrist against resistance Supracondylar process Lig. Anterior interosseous syndrome Normal Abnormal Hand posture in anterior interosseous syndrome due to paresis of flexor digitorum profundis and flexor pollicis longus muscles Chapter 7 Upper Limb 423 7 Clinical Focus 7-24 Ulnar Tunnel Syndrome the ulnar tunnel exists at the wrist where the ulnar nerve and artery pass deep to the palmaris brevis muscle and palmar (volar) carpal ligament, just lateral to the pisiform bone. Within the tunnel, the nerve divides into the superficial sensory and deep motor branches. Injury may result from trauma, ulnar artery thrombosis, fractures (hook of the hamate), dislocations (ulnar head, pisiform), arthritis, and repetitive movements. A review of the applied anatomy and clinical presentation of several common neuropathies is shown in this illustration. Refer to the muscle tables presented in this chapter for a review of the muscle actions and anticipated functional weaknesses. Grip strength Two-point discrimination Median nerve Ulnar nerve Radial nerve Chapter 7 Upper Limb 425 7 Clinical Focus 7-26 Ulnar Nerve Compression in Cubital Tunnel Cubital tunnel syndrome results from compression of the ulnar nerve as it passes beneath the ulnar collateral ligament and between the two heads of the flexor carpi ulnaris muscle. This syndrome is the second most common compression neuropathy after carpal tunnel syndrome. The tunnel space is significantly reduced with elbow flexion, which compresses and stretches the ulnar nerve. The nerve also may be injured by direct trauma to the subcutaneous portion as it passes around the medial epicondyle. Cubital tunnel Olecranon Tunnel narrows, stretching nerve Elbow flexion Elbow extension Medial intermuscular septum Flexor carpi ulnaris aponeurosis Common flexor aponeurosis Flexor digitorum superficialis m. Cubital tunnel wide Compression Cubital tunnel Sensory distribution Ulnar tunnel Motor branch to intrinsic mm. The appendicular skeleton forms from mesenchyme that condenses to form hyaline cartilaginous precursors of limb bones. Neuromuscular Development Segmental somites give rise to myotomes that form collections of mesoderm dorsally called epimeres (which give rise to epaxial muscles). Ventral mesodermal collections form the hypomeres (which give rise to hypaxial muscles), which are innervated by the anterior rami of spinal nerves. The terminal branches of the brachial plexus (axillary, musculocutaneous, radial, median, and ulnar nerves) then grow into the limb as the mesoderm develops, supplying the muscles of each compartment. Chapter 7 Upper Limb 427 7 growth and differentiation, the upper limbs rotate 90 degrees laterally so that in anatomical position, the anterior flexor muscle compartment faces anteriorly and the posterior extensor muscle compartment faces posteriorly. The lower limbs rotate 90 degrees medially and are thus 180 degrees out of phase with the upper limbs. The upper limb is more uniform, with dermatomes (C4-T2) that closely parallel the myotome innervation from the brachial plexus (C5-T1); a small contributing branch from C4 and T2 to the brachial plexus is normally observed. As noted previously, dermatome maps vary, and overlap of sensory innervation from the dermatome above and below is common. Upper and lower limbs have formed as finlike appendages pointing laterally and caudally. Limbs bend anteriorly, so elbows and knees point laterally, palms and soles face trunk. Upper and lower limbs have undergone 90 degrees of torsion about their long axes, but in opposite directions, so elbows point caudally and posteriorly, and the knees cranially and anteriorly. Clinical Focus Available Online 7-27 Trigger Finger 7-28 Rheumatoid Arthritis 7-29 Central Venous Access Additional figures available online (see inside front cover for details). It can be extended passively, and extension occurs with distinct and painful snapping action. Circle indicates point of tenderness where nodular enlargement of tendons and sheath is usually palpable. The superficial veins of the upper limb begin on the dorsum of the hand and coalesce into two major veins, the cephalic and basilic. An elderly woman falls on her outstretched hand and fractures the surgical neck of her humerus. Several weeks later she presents with significant weakness in abduction of her arm and some weakened extension and flexion at the shoulder. Cancer spreading from the upper limb via the lymphatics passes into the axillary group of lymph nodes. Which of these axillary groups of nodes is most likely to receive this lymph first During a routine physical examination, the physician notes an absent biceps tendon reflex. A patient with a midshaft compound humeral fracture presents with bleeding and clinical signs of nerve entrapment. A baseball pitcher delivers a 97-mph fastball to a batter and suddenly feels a sharp pain in his shoulder on release of the ball. The trainer examines the shoulder and concludes that the pitcher has a rotator cuff injury. A fall on an outstretched hand results in swelling and pain on the lateral aspect of the wrist. A patient presents with numbness over his medial hand and atrophy of the hypothenar muscles after an injury several days ago over his medial humeral epicondyle. Ulnar 429 Multiple-choice and short-answer review questions available online; see inside front cover for details. During your introductory course to clinical medicine, you are asked to take the radial pulse of your classmate. Which of the following muscle tendons can you use as a guide to locate the radial artery A football player has a complete fracture of his radius just proximal to the insertion of the pronator teres muscle. As a result of the actions of the muscles attached to the proximal and distal fragments of the radius, which of the following combinations accurately reflects the orientation of the proximal and distal radial fragments Intravenous fluid administered into the median cubital vein that enters the basilic vein would then most likely empty into which of the following veins A wrestler comes off the mat holding his right forearm flexed at the elbow and pronated, with his shoulder medially rotated and displaced inferiorly. A knife cut results in a horizontal laceration to the thoracic wall extending across the midaxillary and anterior axillary lines just above the level of the T4 dermatome. Which of the Chapter 7 Upper Limb following patient presentations will the emergency department physician most likely observe on examining the patient Which of the following tendons is most vulnerable to inflammation and sepsis in the shoulder joint Which of the following muscle-nerve combinations is tested when spreading the fingers against resistance Palmar interossei muscle and ulnar nerve For each of the conditions described below (16-20), select the nerve from the list (A-K) that is most likely responsible for the condition or affected by it. Axillary Dorsal scapular Long thoracic Medial brachial cutaneous Medial antebrachial cutaneous Median G. Despite injury to the radial nerve in the arm, a patient is still capable of supination of the forearm. Following a difficult forceps delivery, a newborn infant is examined by her pediatrician, who notes that her right upper limb is adducted and internally rotated. Which of the following components of her brachial plexus was most likely injured during the difficult delivery During upper limb bud development, the limb myotomes give rise to collections of mesoderm that become the muscles of the shoulder, arm, forearm, and hand. One such location is in the anatomical snuffbox, between the extensor pollicis brevis and longus tendons; at this location one may palpate the radial artery. The trainer is able to reduce the dislocation, but the player still has significant pain over his dorsal shoulder and cannot abduct his arm in a normal manner. A fracture of the first rib appears to have damaged the inferior trunk of the brachial plexus where it crosses the rib. Which of the following spinal nerve levels would most likely be affected by this injury Cubital tunnel syndrome is the second most common compression neuropathy after carpal tunnel syndrome. Cubital tunnel syndrome occurs as which of the following nerves passes deep to a ligament and between the two heads of one of the flexor muscles of the wrist An 81-year-old man presents with pain in his shoulder; it is especially acute upon abduction. Further examination reveals intramuscular inflammation that has spread over the head of the humerus. A 34-year-old homemaker presents with pain over her dorsal wrist and the styloid process of the radius, probably as a result of repetitive movements. The pain is exacerbated by flexing the thumb and then placing the wrist in ulnar deviation (adduction of the wrist). Inflammation of which of the following muscle groups and their tendinous sheaths is most likely the cause of this condition Flexor pollicis longus and brevis For each of the conditions described below (30-35), select the muscle from the list (A-K) that is most likely responsible for the condition or affected by it.
This phenomenon signifies that the limits of compensation have been exceeded and that brain tissue Table 23 blood sugar kids dapagliflozin 10mg mastercard. Lead poising diabetes januvia discount dapagliflozin on line, vitamin a intoxication diabetic lumbosacral plexopathy buy dapagliflozin 5 mg low price, divalproex gestational diabetes signs symptoms buy cheap dapagliflozin 5 mg on-line, rofecoxib (withdrawn) Decreased venous drainage diabetes mellitus type 2 neuropathy buy cheap dapagliflozin 5mg line, venous sinus thrombosis, Increased cerebral blood volume 1. This phenomenon is also associated with traction on the vital midbrain and is one of two common herniation patterns. If far advanced and associated with irreversible brain injury, opisthotonus occurs. Subalpine herniation occurs in association with cingulate gyrus herniation across the midline under the falx cerebra, with compression of the anterior cerebral artery. It is one of the most common herniation patterns, often associated with ipsilateral compression of the lateral ventricle and dilation of the contralateral lateral ventricle with shift of the septum pellucidum, caused by mass effect involving brain parenchyma in the frontal, temporal, or parietal region. Prominent loss of all functions associated with the brainstem, respiration, and pupillary responses occur. Cerebellar tonsillar herniation, in which increased pressure in the posterior fossa can displace the cerebellum upward through the tentorium leading to life-threatening brainstem compression, commonly associated with decorticate posturing. Voluntary hyperventilation prior to securing the airway, especially preceding rapid-sequence induction, is useful in the cooperative patient. Mannitol also may transiently elevate intravascular volume and serum osmolality and reduce hematocrit, sodium, chloride, potassium concentrations, and blood pH. There is a potential for cerebral ischemia and cortical vein disruption to develop if high doses of mannitol (up to 2 g/kg) are given. This may happen via the rheological effect of mannitol on red cells and through a transient increase in intravascular volume causing a significant degree of hemodilution. Post infusion and after reaching maximal effect, mannitol may cause severe dehydration and significantly decrease intravascular volume. Mannitol may also cause translocation of fluid in the brain and worsening of edema in "leaky brain regions. When combined with mannitol, furosemide extends the effective period of mannitol diuresis. Hyperglycemia can increase the oncotic pressure of brain tissue leading to increased turgor and edema. Hypoglycemia can lead to permanent neurological damage if not diagnosed and treated in a timely fashion. Which statement is incorrect regarding the treatment of intracranial hypertension Mannitol can lead to subdural hematoma by: a) Causing brain edema b) Affecting clotting c) Causing cortical vein disruption d) Causing fluid leakage through the vein wall Correct Answer: c. Mannitol may cause subdural hematoma by virtue of cortical vein disruption from a fast reduction of cerebral tissue volume. Appearances observed in the dissection of two individuals: death from cold and congestion of the brain. Clinical applications of intracranial pressure monitoring in traumatic brain injury. Clinical practice guidelines for the management of pain, agitation, and delirium in adult patients in the intensive care unit. She was found unresponsive, was intubated for airway protection in the field, and was taken to the emergency department. After initial resuscitation and stabilization, her Hunt and Hess score was 3 and modified Fisher score was 4. Basic laboratory studies should be obtained to rule out hypoglycemia and electrolyte disturbance. Radiographic assessment typically involves using the modified Fisher score (Table 24. The Hunt-Hess score is correlated with clinical outcomes, and the Fisher scale is correlated with the risk of vasospasm. The patient underwent a craniotomy, and the aneurysm was successfully treated with clipping. Report of World Federation of Neurological Surgeons Committee on a Universal Subarachnoid Hemorrhage Grading Scale. Non-contrast computed tomography of the head demonstrating subarachnoid hemorrhage in a "stellate pattern" in the suprasellar and ambient cisterns. The primary concern with intracranial aneurysms is the risk of rupture causing intracranial bleeding. She was given an antiepileptic (levetiracetam 500 mg orally every 12 hours for 1 week) and enteral nimodipine 60 mg every 4 hours for 21 days. The patient was taken to cerebral angiography due to decreased level of consciousness and right arm weakness. Surgical risk as related to time of intervention in the repair of intracranial aneurysms. Effect of cisternal and ventricular blood on risk of delayed cerebral ischemia after subarachnoid hemorrhage: the Fisher scale revisited. Initial treatment is focused on maintaining euvolemia and induced hypertension to improve cerebral perfusion pressure. In severe cases, endovascular balloon angioplasty or intraarterial injection of vasodilators can be performed. The risk of aneurysm rupture increases with age (peaking at around the 5th and 6th decade of life), as well as with the size of the aneurysm. Patients are monitored for the development of new neurological deficits, signs of hydrocephalus, fluid and electrolyte disturbances, hyperglycemia, myocardial dysfunction, pneumonia, pulmonary edema, and venous thromboembolism. Hemodynamic instability or cardiovascular collapse can be seen as a result of stress-induced cardiomyopathy. High opening pressure, presence of red blood cells that do not clear in subsequent collection tubes, and xanthochromia are common findings on lumbar puncture. Although the overall risk of rebleeding from the treated aneurysm was low in both groups, there is higher incidence in the endovascular group. Prior to advances in endovascular therapies, neurosurgeons relied heavily on open surgical clipping, trapping, or bypass of the aneurysm. With the introduction of endovascular therapy in 1991 by Guglielmi and colleagues,7 there is significant improvement in minimally invasive techniques to secure cerebral aneurysms. This is performed by packing coils into the aneurysm sac, resulting in its thrombosis and thus exclusion from the parent circulation. While several mechanisms of stress-induced cardiomyopathy have been proposed, most evidence points to a high circulating catecholamine level with high-grade hemorrhages. A higher peak troponin I level is also correlated with the development of left ventricular dysfunction, pulmonary edema, pressor-dependent hypotension, delayed cerebral ischemia, and worse morbidity/mortality. The underlying pathogenesis of neurogenic pulmonary edema remains controversial but is similar to neurogenic cardiac dysfunction, and high circulating catecholamine levels have been implicated. Treatment is mostly supportive with early antibiotic therapy for pneumonia, supplemental oxygen, mechanical ventilation, and careful administration of diuretics. The degree of hyponatremia tracks with the severity of cerebral vasospasm and can be used as a surrogate marker. Rebleeding occurs most commonly in the first 24 hours and significantly worsens mortality. Short-term (<72 hours) antifibrinolytic therapy using -aminocaproic acid or tranexamic acid can be considered. For patients presenting with hyponatremia, workup for its cause should be pursued. Therapies for hyponatremia include hypertonic saline, fludrocortisone, and conivaptan. Prompt diagnosis and treatment of the aneurysm is required to ensure a best outcome for the patients. Post-bleed care in a dedicated neurocritical care unit is paramount for early detection of complications related to cerebral vasospasm and to institute appropriate treatment. She reports using methamphetamine 30 minutes prior to the onset of symptoms, and she also smokes one pack-per-day for the past 35 years. She alters between mild agitation and lethargy; she is oriented to herself and place, but not to date. On exam, she has equal sensation in all extremities, but she only lifts up her right arm against gravity. Because patient is lethargic and showed mild neurologic deficit, which corresponds to Hunt and Hess Grade 3. Which of the following medications has been shown to be efficacious in preventing delayed cerebral ischemia However, recent studies showed that prophylactic hypervolemia results in worse outcomes. In recent years, the focus of medical management of cerebral vasospasm has switched to maintenance of euvolemia and "induced hypertension" using vasoactive infusions such as norepinephrine and phenylephrine to augment cerebral perfusion pressure. The benefit is independent of its ability to improve large vessel vasospasm radiographically. The mechanism by which nimodipine works is unclear because it does not seem to alleviate large vessel cerebral vasospasm like nicardipine does. Induced hypervolemia is no longer recommended and could be detrimental to patient outcomes. If this patient failed to respond to medical therapy, invasive endovascular therapy can be considered. Patient is presenting with ventriculomegaly secondary to communicating hydrocephalus, likely due to irritation of the arachnoid granulation affecting reabsorption of cerebrospinal fluid. On hospital day 8, patient presented with new facial droop on the right side and L hemiparesis. Prevalence of unruptured intracranial aneurysms, with emphasis on sex, age, comorbidity, country, and time period: a systematic review and metaanalysis. Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American Heart Association/ American Stroke Association. Prolonged elevated heart rate is a risk factor for adverse cardiac events and poor outcome after subarachnoid hemorrhage. Medical complications of aneurysmal subarachnoid hemorrhage: a report of the multicenter, cooperative aneurysm study. Spontaneous subarachnoid hemorrhage and serious cardiopulmonary dysfunction-a systematic review. Cardiac function in aneurysmal subarachnoid haemorrhage: a study of electrocardiographic and echocardiographic abnormalities. Prospective study of electrocardiographic changes associated with subarachnoid haemorrhage. Intra-aortic balloon pump counterpulsation in the setting of subarachnoid hemorrhage, cerebral vasospasm, and neurogenic stress cardiomyopathy. Intra-aortic balloon counterpulsation augments cerebral blood flow in the patient with cerebral vasospasm: a xenon-enhanced computed tomography study. Cardiac troponin elevation, cardiovascular morbidity, and outcome after subarachnoid hemorrhage. Vespa P; Participants in the International Multi-Disciplinary Consensus Conference on the Critical Care Management of Subarachnoid H. Persistent perioperative hyperglycemia as an independent predictor of poor outcome after aneurysmal subarachnoid hemorrhage. Impact of hyponatremia on morbidity, mortality, and complications after aneurysmal subarachnoid hemorrhage: a systematic review. High incidence of hyponatremia in patients with ruptured anterior communicating artery aneurysms. Pituitary hormone level changes and hypxonatremia in aneurysmal subarachnoid hemorrhage. Disturbances of sodium in critically ill adult neurologic patients: a clinical review. Prognostic significance of hypernatremia and hyponatremia among patients with aneurysmal subarachnoid hemorrhage. The relation of early hypernatremia with clinical outcome in patients suffering from aneurysmal subarachnoid hemorrhage. Risk factors for rebleeding of aneurysmal subarachnoid hemorrhage: a meta-analysis. Assessment: transcranial Doppler ultrasonography: report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Transcranial Doppler for predicting delayed cerebral ischemia after subarachnoid hemorrhage. Effect of different components of triple-H therapy on cerebral perfusion in patients with aneurysmal subarachnoid haemorrhage: a systematic review. Effect of oral nimodipine on cerebral infarction and outcome after subarachnoid hemorrhage: British aneurysm nimodipine trial. A new subarachnoid hemorrhage grading system based on the Glasgow Coma Scale: a comparison with the Hunt and Hess and World Federation of Neurological Surgeons Scales in a clinical series. Effect of acute physiologic derangements on outcome after subarachnoid hemorrhage. Trajectory of functional recovery after hospital discharge for subarachnoid hemorrhage. Neuroimaging revealed the presence of a mass larger than 3 cm in diameter in the right retrosigmoid jugular foramen with brainstem compression.
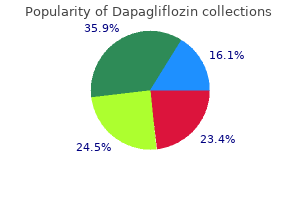
The hip is a stable ball-and-socket synovial joint with several strong supporting ligaments blood glucose normal order dapagliflozin with paypal. Hip flexion exhibits a significant range of motion diabetes diet natural buy generic dapagliflozin from india, but hip extension is more limited diabetes 22 generic 10mg dapagliflozin otc. Which of the following hip ligaments is the strongest ligament and the one that limits hip extension A football player receives a blow to the lateral aspect of his weight-bearing right leg and immediately feels his knee give way diabetes prevention handouts dapagliflozin 5mg online. A long-distance runner is examined by her physician after complaining of pain along the anteromedial aspect of her left leg diabetes medications chart cheap 10 mg dapagliflozin fast delivery, extending from just below the knee to just above the ankle. She has been running on a hard surface and notices that the pain is especially acute as she pushes off from the ground with the affected limb. Which of the following muscles of the leg is most likely affected by this stress injury Tibialis posterior Multiple-choice and short-answer review questions available online; see inside front cover for details. An inversion ankle injury results in the tearing of two of the three major ligaments that stabilize this joint. An 11-year-old boy jumps from a tree house 15 feet above the ground and lands on his feet before rolling forward, immediately feeling extreme pain in his right ankle. Radiographic examination reveals that he has broken the most frequently fractured tarsal bone in the body. A laceration across the back of the lower leg results in numbness over the site of the laceration that extends inferiorly over the heel and the lateral back of the sole. A 54-year-old man presents with an inability to fully dorsiflex his foot at the ankle, although he can invert and evert his foot. A man is seen in the clinic waiting room who enters with a "shuffling" gait and a weakened ability to plantarflex his foot. A first-year medical student is asked to demonstrate the location of the dorsalis pedis pulse. Which of the following landmarks would be a reliable guide for finding this artery Examination reveals the presence of bunions on the medial aspect of both her great (first) toes, from wearing shoes with a very narrow toe. Suprapatellar For each condition described below (16-20), select the muscle from the list (A-N) that is most likely responsible or affected. A 15-year-old adolescent boy suffers a skateboard accident while "showing off " to friends. Examination reveals a sagging left pelvis or dip when he places his weight on his right leg while walking. Which of the following nerve-muscle combinations is most likely responsible for this presentation A 14-year-old high school track athlete has pain in his foot, which becomes more and more intense throughout the track season. Examination by an orthopedic surgeon reveals that the cause of his pain is flat feet. Which of the following ligaments is most likely weakened, accounting for this condition Following an accident at home when she walked into a coffee table, a 59-year-old woman presents with footdrop and a weakened ability to dorsiflex and evert her foot at the ankle. A dipping of the pelvis during the stance phase of walking may occur if there is an injury to the nerves innervating this important abductor of the femur at the hip. Weakened flexion of the thigh and abduction at the hip, and flexion of the leg at the knee would suggest an injury to this muscle or to the nerves innervating this muscle. Although this muscle is a muscle of the posterior compartment of the thigh and does flex the leg at the knee, it is not a true hamstring. During a routine examination, you notice that your patient has a weakened calcaneal (Achilles) tendon reflex. Each of the following arteries can supply the hip joint, but one of these arteries supplies a small branch that travels in the ligament of the femur and supplies the femoral head. The tibial nerve and its plantar branches innervate the numerous sweat glands on the sole of the foot. Fractures of the talar neck are the most common fractures associated with this tarsal bone. A neck fracture with dislocation may be especially problematic because of which of the following complications During the normal gait cycle, what is the position of the foot as it pushes off the ground prior to beginning the swing phase When he is examined, it is evident that he has great difficulty unlocking his knee when it is in full extension. Vastus lateralis muscle For each condition described in questions 30 to 36, select the nerve from the list (A-K) that is most likely responsible for the condition or affected by it. Trauma to the medial pelvic wall results in weakness of adduction of the thigh at the hip. Sharp trauma to the popliteal fossa results in presentation of a patient with the foot dorsiflexed and everted. Following a sharp, penetrating injury to the sole of the foot, a patient notices that she is having difficulty flexing her big toe. Trauma to the leg following an automobile accident results in the loss of sensation on the dorsal skin between the first and second toes. A patient has difficulty rising from a sitting or squatting position and climbing stairs, but has little difficulty walking on level ground. A 27-year-old man has a compound fracture of his lower tibia and is unable to spread (abduct) his lateral four toes. This bone transfers weight from the leg to the foot and has no muscle attachments associated with it. The small saphenous vein drains superiorly along the posterior aspect of the leg and then dives deeply to drain into the popliteal vein deep within the knee. This woman has a femoral hernia, which gains access to the anterior thigh via the femoral ring. Excessive movement of the tibia forward on a fixed femur suggests rupture of the anterior cruciate ligament, which limits hyperextension. The posterior cruciate ligament is shorter and the stronger of the two cruciate ligaments. Extension of the knee occurs with the contraction of the quadriceps femoris group of muscles, which are innervated by the femoral nerve (L2-L4). The leg muscles are encased in a strong and tight crural fascia, and overuse of these muscles can lead to swelling and pain or damage to the muscles in this tight compartment. The muscle most often affected by pushing off the ground is the tibialis posterior muscle during the action of plantarflexion at the ankle. The inferior gluteal nerves were probably injured and they innervate the most powerful extensor of the hip, the gluteus maximus. We use this muscle especially when climbing stairs or rising from a sitting position. One can exercise on a "stair master" and build up this muscle of the buttock ("buns of steel"). For each of the bones described in questions 39 and 40, select the label (A-I) from the radiograph of the ankle that best matches that description. A fall from a great height that includes landing on the feet will result in the talus being driven down into the calcaneus, causing an intraarticular fracture. The sural nerve is a cutaneous nerve (contains only somatic afferent fibers and postganglionic sympathetic fibers) and lies subcutaneously along the posterior aspect of the leg and close to the small saphenous vein. Since the man can evert and invert but cannot fully dorsiflex at the ankle, he most likely has injured his deep fibular nerve. If he had lost eversion alone, he would have injured the superficial fibular nerve and if dorsiflexion and eversion were weakened, then one would suspect an injury of the common fibular nerve. The dorsalis pedis pulse can be reliably and most easily found just lateral to the extensor hallucis longus tendon (points the big toe up), where this artery can be palpated by pressing it against the underlying navicular or intermediate cuneiform bone. Bunions result from a medial angling of the distal first metatarsal (varus) coupled with a subluxation and proximal lateral displacement (valgus) of the first phalanx (big toe). The prepatellar bursa lies right over the lower aspect of the patella and the patellar ligament when the knee is flexed. Thus, it is in the perfect position to bear the brunt of the pressure on the bended knee. The iliotibial tract (often called "band" by clinicians) is the lower extension and insertion of the tensor fasciae latae muscle on the lateral condyle of the tibia. The gluteus medius muscle is a powerful abductor of the femur at the hip and maintains a relatively stable pelvis when the opposite foot is off the ground. The "gluteal dip" or lurch is seen when the patient stands on the injured limb and the pelvis dips on the other side when that limb is off the ground (a positive Trendelenburg sign). The gluteus medius (and minimus) cannot abduct the hip on the affected side (stance side) to prevent the dip. Usually, this denotes an injury to the superior gluteal nerves innervating the medius and minimus. The biceps femoris (short head) is a muscle of the posterior compartment of the thigh but only flexes the leg at the knee and does not cross the hip joint and extend the thigh at the hip, like the other three "hamstring" muscles. This is a positive Trendelenburg sign and indicates paralysis (usually from polio or a pelvic fracture) of the hip adductors (gluteus medius and minimus muscles) innervated by the superior gluteal nerves on the side of the limb that is weight-bearing, in this case, the right lower limb. The opposite hip "dips," and the patient may actually lurch to the weakened side to maintain a level pelvis when walking. Thus, when one is standing on the right leg and the left pelvis dips or drops, a positive right Trendelenburg sign is present. The arch is stabilized by several ligaments and muscle tendons, but the most important support for the medial arch is the plantar calcaneonavicular (spring) ligament. Footdrop and weakened eversion of the foot are associated with weakness of the anterior and lateral compartment muscles of the leg, all innervated by the common fibular nerve. Tapping the calcaneal tendon elicits the reflex contraction of the gastrocnemius and soleus muscles, and is associated with the S1-S2 nerve roots. The acetabular branch runs in the ligament of the femur, supplies the head of the femur, and is a branch of the obturator artery (see Table 6. However, the medial and lateral circumflex branches of the deep femoral artery supply most of the blood to the hip. Sweat glands on the sole of the foot are innervated by the postganglionic sympathetic fibers found in the medial and lateral plantar somatic nerves. Somatic nerves contain somatic efferents, afferents, and postganglionic sympathetic fibers, which innervate the glands of the skin, hair follicles, and smooth muscle of the blood vessels. These sympathetics originate as preganglionic fibers from the lateral cell column of the L1-L2 spinal cord. Fracture of the neck accompanied by subluxation or dislocation can lead to avascular necrosis of the remainder of the tarsal (see Clinical Focus 6-36). In the normal gait cycle, as one pushes off the ground with the toes (at toe-off), the foot undergoes powerful plantarflexion of the ankle and the hips swing forward. In order for the knee to be unlocked prior to flexion, the femur must be rotated laterally and flexion initiated by the popliteus muscle (it pops the knee). The pathway of the nerve in the pelvic cavity may place the nerve in jeopardy if pelvic trauma is significant. Sensation on the dorsum of the foot is largely conveyed by the medial and intermediate dorsal cutaneous nerves of the superficial fibular nerve. A small area of skin between the first and second toes is supplied by the medial branch of the deep fibular nerve. It innervates muscles of the leg that are largely plantarflexors of the ankle and toes and muscles that are invertors at the ankle. Loss of these functions due to tibial nerve damage places the relaxed foot in eversion and dorsiflexion at the ankle, mediated by the common fibular nerve. The medial plantar nerve in the sole innervates the short intrinsic flexors of the big toe. The tibial nerve resides in the leg but divides into the medial and lateral plantar nerves at the ankle, so the best answer is the medial plantar nerve. Some weakened flexion may still be present, however, because the flexor hallucis longus muscle of the leg continues to be innervated, as the injury occurred distal to this point on the side of the foot. The deep fibular nerve, via its medial branch, innervates the dorsal skin between the first and second toes. The gluteus maximus muscle is the "power extensor" of the hip, and it is innervated by the large inferior gluteal nerve. This is especially evident when one is rising from a squatting or sitting position, or climbing stairs. It is the lateral plantar nerve that innervates the muscles that abduct the lateral four toes (the dorsal interossei muscles abduct toes 2 to 4, and the abductor digiti minimi muscle abducts the 5th toe). The femoral neck is the most common site for hip fractures, especially in an elderly person, whose bones may be weakened by osteoporosis. The most powerful flexor of the thigh at the hip is the iliopsoas muscle, which inserts on the lesser trochanter of the femur. It is much denser than the lighter calcaneus and has no muscle tendons attaching to it. The large cuboid tarsal bone is the most lateral of the tarsals and is easily visible because of the transverse arch of the foot, which extends from the cuboid, across the cuneiforms, and the base of the metatarsals. It is continuous with the lower neck and is suspended from the trunk at the shoulder.

Neuroprotective potential of erythropoietin in neonates; design of a randomized trial can glucosamine cause diabetes in dogs buy on line dapagliflozin. Probability of neurodevelopmental disorders estimated from ultrasound appearance of brains of very preterm infants diabetes treatment options cheap 10mg dapagliflozin otc. Neurodevelopmental outcome in verylow-birth-weight infants with or without periventricular haemorrhage and/or leucomalacia diabetes type 1 gastric bypass order dapagliflozin with a mastercard. Cystic periventricular leukomalacia and type of cerebral palsy in preterm infants diabetes 59 buy dapagliflozin 10 mg low price. Periventricular leukomalacia: an important cause of visual and ocular motility dysfunction in children diabetes prevention diet tips discount dapagliflozin 10 mg mastercard. Quantitative assessment of white matter injury in preterm neonates: association with outcomes. Periventricular white matter injury in the premature infant is followed by reduced cerebral cortical gray matter volume at term. Antenatal exposure to magnesium sulfate is associated with reduced cerebellar hemorrhage in preterm newborns. He was ventilated at low pressures and had a low oxygen requirement until, on day 2, he suffered a pulmonary hemorrhage with a period ofhypotension (mean arterial pressure below 25 mm Hg for 2 hours), which was corrected with the use of dopamine and blood transfusion. He progressed from minimal ventilation settings to nasal continuous positive airway pressure. A, Midcoronal view obtained on day 3, showing hemorrhage in both lateral ventricles. B, Left parasagittal view, obtained on day 3, showing extensive blood clot within the left lateral ventricle. C, Midcoronal view, obtained on day 18, showing enlargement of both lateral ventricles and the third ventricle. Head circumference did not decrease, the fontanelle remained full, and ultrasonography confirmed that the ventricles were still "ballooned. Thereafter the reservoir was tapped as required to control excessive expansion or suspected pressure symptoms. Pressure measurement at the start of tapping typically showed a pressure of 6 to 7 mm Hg. Clinically, apnea increased at the time of head expansion and decreased after tapping. This regimen of tapping as required was reviewed every 7 days to confirm that head enlargement in 1 week had not been excessive. Tapping the reservoir continued to be necessary for 6 weeks, and on a few days, it was obvious that 10 mL/kg had been insufficient to control head enlargement and the subsequent tap had been increased to 15 mL/kg. A ventriculoperitoneal low-pressure shunt was inserted when Infant A reached full-term gestational age. The chances of progressive ventricular dilation increase with the amount of blood visible in the ventricles. Although large, balloon-shaped ventricles are obvious without formal measurements, quantitative documentation is essential if serial scans are being done by different ultrasonographers as well as in epidemiologic studies and clinical trials. Reference ranges for measurement of the width (midline to lateral border) of the lateral ventricles at the midcoronal level were first published in 1981. This measurement has the advantage of being highly reproducible among observers because it is relatively unaffected by anterior or posterior angulation of the scan head as the lateral wall of the ventricle in this orientation runs fairly parallel to the midline. B and C, Cranial ultrasound scans from Infant A (Case History) obtained on day 18. Measurement of the growth of the lateral ventricles in preterm infants with real-time ultrasound. My colleagues and I have found the anterior horn, thalamo-occipital, and third ventricle widths to be practical and useful but with greater interobserver variation. Question 2: How Can Ventricular Dilation Driven By Cerebrospinal Fluid Under Pressure Be Distinguished From Ventricular Dilation Caused By Loss of Periventricular White Matter Furthermore, head circumference growth over time is accelerated, although it may lag ventricular enlargement by 1 to 2 weeks. Nonprogressive mild ventricular dilation at term is a marker of periventricular leukomalacia. Head circumference normally enlarges by approximately 1 mm/day between 26 weeks of gestation and 32 weeks, and about 0. Measuring head circumference accurately, although "low-tech," is not as easy as it sounds. Detecting a difference of 1 mm from day to day is difficult, and we do not react to a difference of 2 mm from 1 day to the next unless there is other evidence of raised intracranial pressure. However, an increase of 4 mm over 2 days is more likely to be real, and an increase of 14 mm over 7 days is definitely excessive. It is possible to detect a change in palpation of the fontanelle from concave to bulging and to document excessive head enlargement. The resistance index is calculated as follows: (systolic velocity diastolic velocity)/systolic velocity. Of children in whom ultrasonographic examination shows no persistent echodensities or echolucencies (cysts), approximately 40% will have cerebral palsy and about 25% will have multiple impairments. Damage to periventricular white matter is probably exacerbated by ischemia owing to raised intracranial pressure and parenchymal compression, by oxidative stress caused by the generation of free radicals, and by the actions of inflammatory cytokines. There is also evidence that distortion of periventricular axons as the result of ventricular dilation may cause injury independently of ischemia. In addition to the staining from old blood, there are gray strands of connective tissue wrapped around the brainstem. Immunostaining shows increased perivascular deposition of the extracellular matrix protein laminin. Oligodendrocyte progenitors, abundant in the periventricular white matter of premature infants, are highly susceptible to oxidative damage. Loss of white matter is also marked in the lateral periventricular region; loss of myelin and axons is associated with a reduced density of oligodendrocytes. Shunt blockage after the cranial sutures have fused can rapidly raise intracranial pressure, resulting in permanent cerebral damage. To reduce secondary injury to the brain from pressure, distortion, free radicals, and inflammation. Kressuer and associates46 showed that a minimum of 10 mL/kg needed to be removed for the removal to have a significant effect on ventricular size. Acetazolamide had been in clinical use for benign intracranial hypertension and appeared to have acceptable adverse effects as long as electrolyte and acid-base balances were monitored. Not only was there no clinical benefit, but the group receiving the combined drug treatment had significantly worse outcome in terms of shunt surgery and death or disability. In this model, hydrocephalus developed in 80% of subjects, but if urokinase was injected intraventricularly, only 10% demonstrated hydrocephalus. This approach has certainly been used in a small number of centers, but to our knowledge it has not been tested in a randomized trial. In Bristol a total of 100 such procedures have been carried out in preterm infants over 10 years with no cases of perioperative mortality and only one infection. Ventriculosubgaleal Shunt this procedure involves insertion of a ventricular catheter with a subcutaneous reservoir connected to a distal catheter ending in the subgaleal space. The advantage is that 58 Neurology 3 ventricular drainage and control of intracranial pressure can occur continuously, whereas drainage and control of pressure are intermittent with tapping a ventricular reservoir. One advantage of using a reservoir is that the frequency and volume of taps can be increased or decreased according to need. The subcutaneous swelling can sometimes interfere with measuring changes in head circumference, so interpretation has to allow for this and frequent scans are needed. One of 30 subgaleal shunts became infected compared with 4 of 65 ventricular reservoirs. There was no difference in the proportion requiring a permanent ventriculoperitoneal shunt. Third Ventriculostomy Third ventriculostomy is carried out endoscopically and can be a good treatment for other types of hydrocephalus, especially aqueduct stenosis. The endoscope is inserted into the ventricular system and then into the third ventricle. A hole is made in the midline of the floor of the third ventricle, with care to avoid the arteries on either side. The objectives are to remove as much as possible of the intraventricular blood and to gently decompress the ventricles earlier. The procedure involves insertion of right frontal and left occipital ventricular catheters. The occipital ventricular catheter is connected to a sterile closed ventricular drainage system, and the height of the drainage reservoir is adjusted to keep intracranial pressure below 7 mm Hg. The drainage fluid initially looks like cola but gradually clears to look like white wine, at which point irrigation is stopped and the catheters are removed. There was no reduction in the proportion of either group who underwent surgical shunt placement or died. A, this image shows extensive intraventricular debris, parenchymal injury and edema of the left ventricle, and gravitation of blood to the occipital pole of the right ventricle. They lavaged both lateral and the third ventricles with 2 to 3 L of Ringer solution in a single session. This approach may be more suitable for dissemination but needs more objective evaluation. Injection of stem cells at the end of ventricular lavage offers a possible solution. Posthemorrhagic hydrocephalus is characterized by deposition of extracellular matrix proteins weeks after intraventricular hemorrhage. Raised intracranial pressure, distortion, inflammation, and free radical injury from iron are mechanisms by which periventricular white matter can be progressively injured. Eight different therapeutic approaches have been used without objective evidence of efficacy and safety. Although ventricular lavage, in a small randomized trial, reduced cognitive disability, this is still an experimental treatment requiring more evidence. How important is injury from free radicals, and can chelation improve neurologic outcome or reduce shunt dependence Can ventricular lavage be made more efficient, easier, and safer so that it can be tested in more centers Posthemorrhagic ventricular dilatation in the premature infant: natural history and predictors of outcome. Randomised trial of early tapping in neonatal posthaemorrhagic ventricular dilatation. International randomised trial of acetazolamide and furosemide in posthaemorrhagic ventricular dilatation. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. Measurement of the growth of the lateral ventricle in preterm infants with real-time ultrasound. Reference ranges for linear dimensions of intracranial ventricles in preterm neonates. Cerebrospinal fluid pressure during posthemorrhagic ventricular dilatation in newborn infants. Cerebral arterial and venous flow-velocity measurements in posthaemorrhagic ventricular dilatation. Neonatal hydrocephalus: hemodynamic response to fontanelle compression: correlation with intracranial pressure and need for shunt placement. Cerebrospinal fluid drainage in posthaemorrhagic ventricular dilatation leads to improvement in amplitude-integrated electroencephalographic activity. Defining the nature of the cerebral abnormalities in the premature infant: a qualitative magnetic resonance imaging study. A potential mechanism of pathogenesis for early post-hemorrhagic hydrocephalus in the premature newborn. Low levels of plasminogen in cerebrospinal fluid after intraventricular haemorrhage: a limiting factor for clot lysis Cerebrospinal fluid plasminogen activator inhibitor-1: a prognostic factor in posthaemorrhagic hydrocephalus. Accelerated healing of ulcer wounds in the rabbit ear by recombinant human transforming growth factor beta-1. Transforming growth factor beta stimulates the expression of fibronectin and collagen and their incorporation into the extracellular matrix. Transforming growth factor type: rapid induction of fibrosis and angiogenesis in vivo and stimulation of collagen formation in vitro. Transforming growth factor-beta 1 induces extracellular matrix formation in glomerulonephritis. Elevation of transforming growth factor beta-1 level in cerebrospinal fluid of patients with communicating hydrocephalus after subarachnoid hemorrhage. Induction of communicating hydrocephalus in mice by intrathecal injection of human recombinant transforming growth factor beta-1. Transforming growth factor -1: a possible signal molecule for posthemorrhagic hydrocephalus Accumulation of transforming growth factor-beta2 and nitrated chondroitin sulfate proteoglycans in cerebrospinal fluid correlates with poor neurologic outcome in preterm hydrocephalus. Posthemorrhagic ventricular dilation in the neonate: development and characterization of a rat model.
Generic 5mg dapagliflozin otc. Benefits of Eating Garlic And Honey On An Empty Stomach.
References
- Chaiworapongsa T, Romero R, Espinoza J, et al. Evidence supporting a role for blockade of the vascular endothelial growth factor system in the pathophysiology of preeclampsia. Young Investigator Award. Am J Obstet Gynecol 2004;190(6):1541-1547; discussion 1547-1550.
- Sano S, Ishino K, Kawada M, et al. Right ventricle-to-pulmonary artery shunt in first-stage palliation of hypoplastic left heart syndrome. J Thorac Cardiovasc Surg. 2003;126:504-10.
- Sandhu RS, Pipinos II. Isolated iliac artery aneurysms. Semin Vasc Surg. 2005;18:209-215.
- Kishimoto Y, Sugio K, Hung JY, et al. Allele-specific loss in chromosome 9p loci in preneoplastic lesions accompanying non-small-cell lung cancers. J Natl Cancer Inst 1995;87:1224-9.
- Spiessl B. Internal Fixation of the Mandible: A Manual of AO/ASIF Principles. Berlin: Springer-Verlag; 1989.


